Abstract
Aims
To investigate the impact of baseline kidney function on outcomes following comprehensive cardiac rehabilitation (CR) in patients with heart failure (HF).
Methods
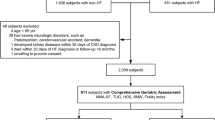
We reviewed a total of 3,727 patients who were admitted for HF treatment. Estimated glomerular filtration rate (eGFR), quadriceps strength (QS), and 6-min walk distance (6MWD) were measured at hospital discharge as a baseline and 5 months thereafter in participants of outpatient comprehensive CR. The association between outpatient CR participation and all-cause events was evaluated using propensity score-matched analysis in subgroups across eGFR stages. The changes in QS and 6MWD following 5-month CR were compared between eGFR stages.
Results
Out of the studied patients, 1585 (42.5%) participated in outpatient CR. After propensity matching for clinical confounders, 2680 patients were included for analysis (pairs of n = 1340 outpatient CR participants and nonparticipants). The participation in outpatient CR was significantly associated with low clinical events in subgroups of eGFR ≥ 60 [hazard ratio (HR): 0.65, 95% confidence interval (CI): 0.51–0.84] and eGFR 45–60 (HR: 0.71, 95% CI: 0.55–0.92), but not in eGFR 30–45 (HR: 0.83, 95% CI: 0.64–1.08) and eGFR < 30 (HR: 0.88, 95% CI: 0.69–1.12). QS and 6MWD were significantly higher after 5-month CR than those at baseline (P < 0.001, respectively), but lower baseline eGFR correlated with lower changes in QS and 6MWD (trend P < 0.001, respectively).
Conclusions
Although low baseline kidney function attenuates the outcomes of CR, outpatient CR seems to be associated with a better prognosis and positive change in physical function in HF patients with low kidney function.
Graphic abstract








Similar content being viewed by others
References
Mentz RJ, Kelly JP, Von Lueder TG et al (2014) Noncardiac comorbidities in heart failure with reduced versus preserved ejection fraction. J Am Coll Cardiol 64:2281–2293
Streng KW, Nauta JF, Hillege HL et al (2018) Non-cardiac comorbidities in heart failure with reduced, mid-range and preserved ejection fraction. Int J Cardiol 271:132–139
Damman K, Testani JM (2015) The kidney in heart failure: an update. Eur Heart J 36:1437–1444
House AA, Wanner C, Sarnak MJ et al (2019) Heart failure in chronic kidney disease: conclusions from a Kidney Disease: Improving Global Outcomes (KDIGO) Controversies Conference. Kidney Int 95:1304–1317
Schardong J, MaZ M, Plentz RDM (2018) Muscle atrophy in chronic kidney disease. Adv Exp Med Biol 1088:393–412
Adams GR, Vaziri ND (2006) Skeletal muscle dysfunction in chronic renal failure: effects of exercise. Am J Physiol Renal Physiol 290:F753-761
Taylor RS, Long L, Mordi IR et al (2019) Exercise-based rehabilitation for heart failure: cochrane systematic review, meta-analysis, and trial sequential analysis. JACC Heart Fail 7:691–705
O’connor CM, Whellan DJ, Lee KL et al (2009) Efficacy and safety of exercise training in patients with chronic heart failure: HF-ACTION randomized controlled trial. JAMA 301:1439–1450
Ambrosy AP, Mulder H, Coles A et al (2018) Renal function and exercise training in ambulatoryheart failure patients with a reduced ejection fraction. Am J Cardiol 122:999–1007
Saitoh M, Takahashi T, Sakurada K et al (2013) Factors determining achievement of early postoperative cardiac rehabilitation goal in patients with or without preoperative kidney dysfunction undergoing isolated cardiac surgery. J Cardiol 61:299–303
Izawa H, Yoshida T, Ikegame T et al (2019) Standard cardiac rehabilitation program for heart failure. Circ J 83:2394–2398
Chen YJ, Sung SH, Cheng HM et al (2017) Performance of AHEAD score in an asian cohort of acute heart failure with either preserved or reduced left ventricular systolic function. J Am Heart Assoc. https://doi.org/10.1161/JAHA.116.004297
Kamiya K, Masuda T, Tanaka S et al (2015) Quadriceps strength as a predictor of mortality in coronary artery disease. Am J Med 128:1212–1219
Laboratories ATSCOPSFCPF (2002) ATS statement: guidelines for the six-minute walk test. Am J Respir Crit Care Med 166:111–117
Group JCSJW (2014) Guidelines for rehabilitation in patients with cardiovascular disease (JCS 2012). Circ J 78:2022–2093
Persinger R, Foster C, Gibson M et al (2004) Consistency of the talk test for exercise prescription. Med Sci Sports Exerc 36:1632–1636
Piepoli MF, Conraads V, Corra U et al (2011) Exercise training in heart failure: from theory to practice. A consensus document of the Heart Failure Association and the European Association for Cardiovascular Prevention and Rehabilitation. Eur J Heart Fail 13:347–357
Kamiya K, Sato Y, Takahashi T et al (2020) Multidisciplinary cardiac rehabilitation and long-term prognosis in patients with heart failure. Circ Heart Fail 13:006798
Bouillon K, Batty GD, Hamer M et al (2013) Cardiovascular disease risk scores in identifying future frailty: the Whitehall II prospective cohort study. Heart 99:737–742
Roshanravan B, Gamboa J, Wilund K (2017) Exercise and CKD: skeletal muscle dysfunction and practical application of exercise to prevent and treat physical impairments in CKD. Am J Kidney Dis 69:837–852
Del Buono MG, Arena R, Borlaug BA et al (2019) Exercise intolerance in patients with heart failure: JACC state-of-the-art review. J Am Coll Cardiol 73:2209–2225
Nakamura T, Kamiya K, Hamazaki N et al (2020) Quadriceps strength and mortality in older patients with heart failure. Can J Cardiol 37(3):476–483
Sietsema KE, Amato A, Adler SG et al (2004) Exercise capacity as a predictor of survival among ambulatory patients with end-stage renal disease. Kidney Int 65:719–724
Reeves GR, Whellan DJ, O’connor CM et al (2017) A novel rehabilitation intervention for older patients with acute decompensated heart failure: the REHAB-HF pilot study. JACC Heart Fail 5:359–366
Hamazaki N, Kamiya K, Yamamoto S et al (2020) Changes in respiratory muscle strength following cardiac rehabilitation for prognosis in patients with heart failure. J Clin Med 9(4):952
Colombo PC, Ganda A, Lin J et al (2012) Inflammatory activation: cardiac, renal, and cardio-renal interactions in patients with the cardiorenal syndrome. Heart Fail Rev 17:177–190
Hirai DM, Musch TI, Poole DC (2015) Exercise training in chronic heart failure: improving skeletal muscle O2 transport and utilization. Am J Physiol Heart Circ Physiol 309:H1419-1439
Taylor RS, Walker S, Smart NA et al (2018) Impact of exercise-based cardiac rehabilitation in patients with heart failure (ExTraMATCH II) on mortality and hospitalisation: an individual patient data meta-analysis of randomised trials. Eur J Heart Fail 20:1735–1743
Mudge AM, Denaro CP, Scott AC et al (2018) Addition of supervised exercise training to a post-hospital disease management program for patients recently hospitalized with acute heart failure: the EJECTION-HF randomized phase 4 trial. JACC Heart Fail 6:143–152
Kaminsky LA, Tuttle MS (2015) Functional assessment of heart failure patients. Heart Fail Clin 11:29–36
Funding
This work was supported by Japan Society for the Promotion of Science Grant-in-Aid (JSPS KAKENHI Grant Number JP19K1922).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors report no conflict of interest related to this manuscript.
Ethical approval
This study protocol was approved by the Kitasato Institute Clinical Research Review Board (KMEO B18-075).
Informed consent
All patients provided informed consent.
Supplementary Information
Below is the link to the electronic supplementary material.
392_2021_1875_MOESM1_ESM.docx
Comparisons between clinical variables before and after the 5-month CR. Orange bars indicate baseline; green bars indicate after 5-month CR. Data, mean and standard error. BMI body mass index, BNP brain natriuretic peptide, CR cardiac rehabilitation, eGFR estimated glomerular filtration rate, QS quadriceps strength, 6MWD 6-min walk distance (TIF 981 kb)
Rights and permissions
About this article
Cite this article
Hamazaki, N., Kamiya, K., Yamamoto, S. et al. Associations between kidney function and outcomes of comprehensive cardiac rehabilitation in patients with heart failure. Clin Res Cardiol 111, 253–263 (2022). https://doi.org/10.1007/s00392-021-01875-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-021-01875-2