Abstract
Background
Estimated plasma volume status (ePVS) has diagnostic and prognostic value in patients with heart failure (HF). However, it remains unclear which congestion markers (i.e., biological, imaging, and hemodynamic markers) are preferentially associated with ePVS. In addition, there is evidence of sex differences in both the hematopoietic process and myocardial structure/function.
Method and results
Patients with significant dyspnea (NYHA ≥ 2) underwent echocardiography and lung ultrasound within 4 h prior to cardiac catheterization. Patients were divided according to tertiles based on sex-specific ePVS thresholds calculated from hemoglobin and hematocrit measurements using Duarte’s formula. Among the 78 included patients (median age 74.5 years; males 69.2%; HF 48.7%), median ePVS was 4.1 (percentile25–75 = 3.7–4.9) mL/g in males (N = 54) and 4.8 (4.4–5.3) mL/g in females (N = 24). Patients with the highest ePVS had more frequently HF, higher NT-proBNP, larger left atrial volume, and higher E/e’ (all p values < 0.05), but no difference in inferior vena cava diameter or pulmonary congestion assessed by lung ultrasound (all p values > 0.10). In multivariable analysis, higher E/e’ and lower diastolic blood pressure were significantly associated with increased ePVS. The association between ePVS and congestion variables was not sex-dependent except for left-ventricular end-diastolic pressure, which was only correlated with ePVS in females (Spearman Rho = 0.53, p < 0.01 in females and Spearman Rho = − 0.04, p = 0.76 in males; pinteraction = 0.08).
Conclusion
ePVS is associated with E/e’ regardless of sex, while only associated with invasively measured left-ventricular end-diastolic pressure in females. These results suggest that ePVS is preferably associated with left-sided hemodynamic markers of congestion.
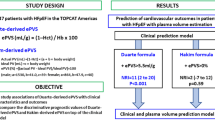
Graphical abstract



Similar content being viewed by others
References
Miller WL (2016) Fluid volume overload and congestion in heart failure: time to reconsider pathophysiology and how volume is assessed. Circ Heart Fail 9:e002922
Francis GS, Benedict C, Johnstone DE, Kirlin PC, Nicklas J, Liang CS, Kubo SH, Rudin-Toretsky E, Yusuf S (1990) Comparison of neuroendocrine activation in patients with left ventricular dysfunction with and without congestive heart failure. A substudy of the Studies of Left Ventricular Dysfunction (SOLVD). Circulation 82:1724–1729
Duarte K, Monnez JM, Albuisson E, Pitt B, Zannad F, Rossignol P (2015) Prognostic value of estimated plasma volume in heart failure. JACC Heart Fail 3:886–893
Ling HZ, Flint J, Damgaard M, Bonfils PK, Cheng AS, Aggarwal S, Velmurugan S, Mendonca M, Rashid M, Kang S, Papalia F, Weissert S, Coats CJ, Thomas M, Kuskowski M, Cohn JN, Woldman S, Anand IS, Okonko DO (2015) Calculated plasma volume status and prognosis in chronic heart failure. Eur J Heart Fail 17:35–43
Kobayashi M, Rossignol P, Ferreira JP, Aragao I, Paku Y, Iwasaki Y et al (2019) Prognostic value of estimated plasma volume in acute heart failure in three cohort studies. Clin Res Cardiol 108(5):549–561
Chouihed T, Rossignol P, Bassand A, Duarte K, Kobayashi M, Jaeger D et al (2019) Diagnostic and prognostic value of plasma volume status at emergency department admission in dyspneic patients: results from the PARADISE cohort. Clin Res Cardiol 108(5):563–573
Fudim M, Miller WL (2018) Calculated estimates of plasma volume in patients with chronic heart failure-comparison with measured volumes. J Card Fail 24(9):553–560
Martens P, Nijst P, Dupont M, Mullens W (2019) The optimal plasma volume status in heart failure in relation to clinical outcome. J Card Fail 25(4):240–248
Dekkers CCJ, Sjostrom CD, Greasley PJ, Cain V, Boulton DW, Heerspink HJL (2019) Effects of the sodium-glucose co-transporter-2 inhibitor dapagliflozin on estimated plasma volume in patients with type 2 diabetes. Diabetes Obes Metab 21(12):2667–2673
Greene SJ, Gheorghiade M, Vaduganathan M, Ambrosy AP, Mentz RJ, Subacius H, Maggioni AP, Nodari S, Konstam MA, Butler J (2013) Filippatos G and investigators ET Haemoconcentration, renal function, and post-discharge outcomes among patients hospitalized for heart failure with reduced ejection fraction: insights from the EVEREST trial. Eur J Heart Fail. 15:1401–1411
Testani JM, Chen J, McCauley BD, Kimmel SE, Shannon RP (2010) Potential effects of aggressive decongestion during the treatment of decompensated heart failure on renal function and survival. Circulation 122:265–272
van der Meer P, Postmus D, Ponikowski P, Cleland JG, O'Connor CM, Cotter G, Metra M, Davison BA, Givertz MM, Mansoor GA, Teerlink JR, Massie BM, Hillege HL, Voors AA (2013) The predictive value of short-term changes in hemoglobin concentration in patients presenting with acute decompensated heart failure. J Am Coll Cardiol 61:1973–1981
Murphy WG (2014) The sex difference in haemoglobin levels in adults-mechanisms, causes, and consequences. Blood Rev 28:41–47
Beale AL, Nanayakkara S, Segan L, Mariani JA, Maeder MT, van Empel V, Vizi D, Evans S, Lam CSP, Kaye DM (2019) Sex differences in heart failure with preserved ejection fraction pathophysiology: a detailed invasive hemodynamic and echocardiographic analysis. JACC Heart Fail 7:239–249
Beale AL, Meyer P, Marwick TH, Lam CSP, Kaye DM (2018) Sex differences in cardiovascular pathophysiology: Why women are overrepresented in heart failure with preserved ejection fraction. Circulation 138:198–205
Hubert A, Girerd N, Le Breton H, Galli E, Latar I, Fournet M, Mabo P, Schnell F, Leclercq C, Donal E (2019) Diagnostic accuracy of lung ultrasound for identification of elevated left ventricular filling pressure. Int J Cardiol 281:62–68
Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JG, Coats AJ, Falk V, Gonzalez-Juanatey JR, Harjola VP, Jankowska EA, Jessup M, Linde C, Nihoyannopoulos P, Parissis JT, Pieske B, Riley JP, Rosano GM, Ruilope LM, Ruschitzka F, Rutten FH, van der Meer P, Authors/Task Force M, and Document R (2016) 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur J Heart Fail 18:891–975
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF 3rd, Feldman HI, Kusek JW, Eggers P, Van Lente F, Greene T, Coresh J (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150:604–612
Nagueh SF, Smiseth OA, Appleton CP, Byrd BF 3rd, Dokainish H, Edvardsen T, Flachskampf FA, Gillebert TC, Klein AL, Lancellotti P, Marino P, Oh JK, Popescu BA, Waggoner AD (2016) Recommendations for the evaluation of left ventricular diastolic function by echocardiography: an update from the american society of echocardiography and the european association of cardiovascular imaging. J Am Soc Echocardiogr 29:277–314
Picano E, Frassi F, Agricola E, Gligorova S, Gargani L, Mottola G (2006) Ultrasound lung comets: a clinically useful sign of extravascular lung water. J Am Soc Echocardiogr 19:356–363
Hakim RM (2001) Plasmapheresis. In: Daugirdas JT, Blake PG, Ing TS (eds) Handbook of dialysis, 3rd edn. Lippincott Williams and Wilkins, Philadelphia, p 236
Platz E, Lattanzi A, Agbo C, Takeuchi M, Resnic FS, Solomon SD, Desai AS (2012) Utility of lung ultrasound in predicting pulmonary and cardiac pressures. Eur J Heart Fail 14:1276–1284
Sharifov OF, Schiros CG, Aban I, Denney TS, Gupta H (2016) Diagnostic accuracy of tissue doppler index E/e' for evaluating left ventricular filling pressure and diastolic dysfunction/heart failure with preserved ejection fraction: a systematic review and meta-analysis. J Am Heart Assoc 5
Nagueh SF (2020) Left ventricular diastolic function: understanding pathophysiology, diagnosis, and prognosis with echocardiography. JACC Cardiovasc Imaging 13(1 Pt 2):228–244
Shah AM, Claggett B, Kitzman D, Biering-Sorensen T, Jensen JS, Cheng S, Matsushita K, Konety S, Folsom AR, Mosley TH, Wright JD, Heiss G, Solomon SD (2017) Contemporary assessment of left ventricular diastolic function in older adults: the atherosclerosis risk in communities study. Circulation 135:426–439
Dokainish H, Zoghbi WA, Lakkis NM, Ambriz E, Patel R, Quinones MA, Nagueh SF (2005) Incremental predictive power of B-type natriuretic peptide and tissue Doppler echocardiography in the prognosis of patients with congestive heart failure. J Am Coll Cardiol 45:1223–1226
Neeland IJ, Drazner MH, Berry JD, Ayers CR, deFilippi C, Seliger SL, Nambi V, McGuire DK, Omland T, de Lemos JA (2013) Biomarkers of chronic cardiac injury and hemodynamic stress identify a malignant phenotype of left ventricular hypertrophy in the general population. J Am Coll Cardiol. 61:187–195
Girerd N, Seronde MF, Coiro S, Chouihed T, Bilbault P, Braun F, Kenizou D, Maillier B, Nazeyrollas P, Roul G, Fillieux L, Abraham WT, Januzzi J Jr, Sebbag L, Zannad F, Mebazaa A, Rossignol P (2018) Integrative assessment of congestion in heart failure throughout the patient journey. JACC Heart Fail 6:273–285
Rossignol P, Menard J, Fay R, Gustafsson F, Pitt B, Zannad F (2011) Eplerenone survival benefits in heart failure patients post-myocardial infarction are independent from its diuretic and potassium-sparing effects. Insights from an EPHESUS (Eplerenone Post-Acute Myocardial Infarction Heart Failure Efficacy and Survival Study) substudy. J Am Coll Cardiol 58:1958–1966
Grodin JL, Philips S, Mullens W, Nijst P, Martens P, Fang JC, Drazner MH, Tang WHW, Pandey A (2019) Prognostic implications of plasma volume status estimates in heart failure with preserved ejection fraction: insights from TOPCAT. Eur J Heart Fail 21(5):634–642
Gelman S (2008) Venous function and central venous pressure: a physiologic story. Anesthesiology 108:735–748
Galderisi M, Anderson KM, Wilson PW, Levy D (1991) Echocardiographic evidence for the existence of a distinct diabetic cardiomyopathy (the Framingham Heart Study). Am J Cardiol 68:85–89
Redfield MM, Jacobsen SJ, Borlaug BA, Rodeheffer RJ, Kass DA (2005) Age- and gender-related ventricular-vascular stiffening: a community-based study. Circulation 112:2254–2262
Najjar SS, Schulman SP, Gerstenblith G, Fleg JL, Kass DA, O'Connor F, Becker LC, Lakatta EG (2004) Age and gender affect ventricular-vascular coupling during aerobic exercise. J Am Coll Cardiol 44:611–617
Daniels LB, Maisel AS (2007) Natriuretic peptides. J Am Coll Cardiol 50:2357–2368
Rueda-Ochoa OL, Smiderle-Gelain MA, Rizopoulos D, Dhana K, van den Berge JK, Echeverria LE, Ikram MA, Deckers JW, Franco OH, Kavousi M (2019) Risk factors for longitudinal changes in left ventricular diastolic function among women and men. Heart 105(18):1414–1422
Flint N, Kaufman N, Gal-Oz A, Margolis G, Topilsky Y, Keren G, Shacham Y (2017) Echocardiographic correlates of left ventricular filling pressures and acute cardio-renal syndrome in ST segment elevation myocardial infarction patients. Clin Res Cardiol 106:120–126
Ambrosy AP, Cerbin LP, Armstrong PW, Butler J, Coles A, DeVore AD, Dunlap ME, Ezekowitz JA, Felker GM, Fudim M, Greene SJ, Hernandez AF, O'Connor CM, Schulte P, Starling RC, Teerlink JR, Voors AA, Mentz RJ (2017) Body weight change during and after hospitalization for acute heart failure: patient characteristics, markers of congestion, and outcomes: findings from the ASCEND-HF Trial. JACC Heart Fail 5:1–13
Anker SD, Negassa A, Coats AJS, Afzal R, Poole-Wilson PA, Cohn JN, Yusuf S (2003) Prognostic importance of weight loss in chronic heart failure and the effect of treatment with angiotensin-converting-enzyme inhibitors: an observational study. The Lancet 361:1077–1083
Acknowledgements
The Nancy team is supported by the RHU Fight-HF, a public grant overseen by the French National Research Agency (ANR) as part of the second “Investissements d’Avenir” program (reference: ANR-15-RHUS-0004), by the French PIA project “Lorraine Université d’Excellence” (reference: ANR-15-IDEX-04-LUE), the ANR FOCUS-MR (reference: ANR-15-CE14-0032-01), ERA-CVD EXPERT (reference: ANR-16-ECVD-0002-02), Contrat de Plan Etat Lorraine IT2MP and FEDER Lorraine.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
N.G. reports honoraria from Novartis and Boehringer. P.R. reports grants and personal fees from AstraZeneca, grants and personal fees from Bayer, grants and personal fees from CVRx, personal fees from Fresenius, grants and personal fees from Novartis, personal fees from Grunenthal, personal fees from Servier, personal fees from Stealth Peptides, personal fees from Vifor Fresenius Medical Care Renal Pharma, personal fees from Idorsia, personal fees from NovoNordisk, personal fees from Ablative Solutions, personal fees from G3P, personal fees from Corvidia, personal fees from Relypsa, outside the submitted work; and Cofounder: CardioRenal, a company developing a telemonitoring loop in heart failure (including potassium measurements). All other authors have no conflicts to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kobayashi, M., Huttin, O., Donal, E. et al. Association of estimated plasma volume status with hemodynamic and echocardiographic parameters. Clin Res Cardiol 109, 1060–1069 (2020). https://doi.org/10.1007/s00392-020-01599-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-020-01599-9