Abstract
Aims
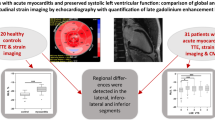
Lake Louise Criteria (LLC) are time-dependent and some acute myocarditis (AM) with preserved left ventricular ejection fraction (LVEF) could be missed, due to the limited accessibility of Cardiac Magnetic Resonance (CMR). We aimed to assess the potential value of cardiac strain measured by feature tracking (FT) imaging in this population.
Methods and results
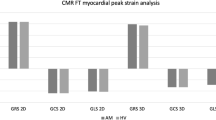
Eighty-three patients with clinically suspected AM and normal LVEF were divided into 39 “confirmed AM” (positive LLC) and 44 “suspected AM” (negative LLC). An age and gender-matched sample of 42 normal subjects underwent CMR. In all groups, FT-derived biventricular strains and STE- global longitudinal strain (GLS) were assessed, being regularly measurable. Strain values < 5th percentile of the control group were considered abnormal. “Suspected” and “confirmed” AM were similar, except for medium time of CMR evaluation (5.2 vs 1 months from presentation, respectively; p = 0.004). Compared to healthy controls, both “suspected” and “confirmed” AM showed significantly impaired strain values. LV-global circumferential strain (GCS), right ventricular GCS and LV-GLS were abnormal in 15.4% and 15.9%, 20.5% and 15.9%, 7.7% and 9.1% in “confirmed” and “suspected” AM, respectively. STE analysis confirmed the results on LV-GLS, however a weak correlation emerged between STE and CMR-FT LV-GLS (p = 0.08).
Conclusions
Compared to STE, CMR-FT analysis provided a more comprehensive and complementary biventricular strain evaluation that resulted similar in “confirmed” and “suspected” AM with normal LVEF. Conversely, mostly biventricular GCS was significantly reduced in up to 20% of patients, compared to healthy controls.
Graphic abstract




Similar content being viewed by others
References
Trachtenberg BH, Hare JM (2017) Inflammatory cardiomyopathic syndromes. Circ Res 121:803–818. https://doi.org/10.1161/CIRCRESAHA.117.310221
Cooper LT, Baughman KL, Feldman AM, Frustaci A, Jessup M, Kuhl U, Levine GN, Narula J, Starling RC, Towbin J, Virmani R (2007) The role of endomyocardial biopsy in the management of cardiovascular disease: a scientific statement from the American Heart Association, the American College of Cardiology, and the European Society of Cardiology. Endorsed by the Heart Failure Society. J Am Coll Cardiol 50:1914–1931. https://doi.org/10.1016/j.jacc.2007.09.008
Francone M, Chimenti C, Galea N, Scopelliti F, Verardo R, Galea R, Carbone I, Catalano C, Fedele F, Frustaci A (2014) CMR sensitivity varies with clinical presentation and extent of cell necrosis in biopsy-proven acute myocarditis. JACC Cardiovasc Imaging 7:254–263. https://doi.org/10.1016/j.jcmg.2013.10.011
De Cobelli F, Pieroni M, Esposito A, Chimenti C, Belloni E, Mellone R, Canu T, Perseghin G, Gaudio C, Maseri A, Frustaci A, Del Maschio A (2006) Delayed Gadolinium-enhanced cardiac magnetic resonance in patients with chronic myocarditis presenting with heart failure or recurrent arrhythmias. J Am Coll Cardiol. https://doi.org/10.1016/j.jacc.2005.11.067
Ferreira VM, Schulz-Menger J, Holmvang G, Kramer CM, Carbone I, Sechtem U, Kindermann I, Gutberlet M, Cooper LT, Liu P, Friedrich MG (2018) Cardiovascular magnetic resonance in nonischemic myocardial inflammation: expert recommendations. J Am Coll Cardiol 72:3158–3176. https://doi.org/10.1016/j.jacc.2018.09.072
Radunski UK, Lund GK, Säring D, Bohnen S, Stehning C, Schnackenburg B, Avanesov M, Tahir E, Adam G, Blankenberg S, Muellerleile K (2017) T1 and T2 mapping cardiovascular magnetic resonance imaging techniques reveal unapparent myocardial injury in patients with myocarditis. Clin Res Cardiol. https://doi.org/10.1007/s00392-016-1018-5
Lurz P, Eitel I, Adam J, Steiner J, Grothoff M, Desch S, Fuernau G, de Waha S, Sareban M, Luecke C, Klingel K, Kandolf R, Schuler G, Gutberlet M, Thiele H (2012) Diagnostic performance of CMR imaging compared with EMB in patients with suspected myocarditis. JACC Cardiovasc Imaging 5:513–524. https://doi.org/10.1016/j.jcmg.2011.11.022
Heermann P, Fritsch H, Koopmann M, Sporns P, Paul M, Heindel W, Schulze-Bahr E, Schülke C (2019) Biventricular myocardial strain analysis using cardiac magnetic resonance feature tracking (CMR-FT) in patients with distinct types of right ventricular diseases comparing arrhythmogenic right ventricular cardiomyopathy (ARVC), right ventricular outflow-t. Clin Res Cardiol. https://doi.org/10.1007/s00392-019-01450-w
Bietenbeck M, Florian A, Shomanova Z, Klingel K, Yilmaz A (2017) Novel CMR techniques enable detection of even mild autoimmune myocarditis in a patient with systemic lupus erythematosus. Clin Res Cardiol 106:560–563
Baron T, Berglund L, Hedin E-M, Flachskampf FA (2019) Test-retest reliability of new and conventional echocardiographic parameters of left ventricular systolic function. Clin Res Cardiol 108:355–365. https://doi.org/10.1007/s00392-018-1363-7
Zamorano JL, Lancellotti P, Rodriguez Munoz D, Aboyans V, Asteggiano R, Galderisi M, Habib G, Lenihan DJ, Lip GYH, Lyon AR, Lopez Fernandez T, Mohty D, Piepoli MF, Tamargo J, Torbicki A, Suter TM (2016) 2016 ESC Position Paper on cancer treatments and cardiovascular toxicity developed under the auspices of the ESC Committee for Practice Guidelines: the Task Force for cancer treatments and cardiovascular toxicity of the European Society of Cardiology (ESC). Eur Heart J 37:2768–2801. https://doi.org/10.1093/eurheartj/ehw211
Sawaya H, Sebag IA, Plana JC, Januzzi JL, Ky B, Tan TC, Cohen V, Banchs J, Carver JR, Wiegers SE, Martin RP, Picard MH, Gerszten RE, Halpern EF, Passeri J, Kuter I, Scherrer-Crosbie M (2012) Assessment of echocardiography and biomarkers for the extended prediction of cardiotoxicity in patients treated with anthracyclines, taxanes, and trastuzumab. Circ Cardiovasc Imaging. https://doi.org/10.1161/CIRCIMAGING.112.973321
Negishi K, Negishi T, Hare JL, Haluska BA, Plana JC, Marwick TH (2013) Independent and incremental value of deformation indices for prediction of trastuzumab-induced cardiotoxicity. J Am Soc Echocardiogr 26:493–498. https://doi.org/10.1016/j.echo.2013.02.008
Laufer-Perl M, Arnold JH, Mor L, Amrami N, Derakhshesh M, Moshkovits Y, Sadeh B, Arbel Y, Topilsky Y, Rozenbaum Z (2019) The association of reduced global longitudinal strain with cancer therapy-related cardiac dysfunction among patients receiving cancer therapy. Clin Res Cardiol. https://doi.org/10.1007/s00392-019-01508-9
Kostakou PM, Kostopoulos VS, Tryfou ES, Giannaris VD, Rodis IE, Olympios CD, Kouris NT (2018) Subclinical left ventricular dysfunction and correlation with regional strain analysis in myocarditis with normal ejection fraction. A new diagnostic criterion. Int J Cardiol 259:116–121. https://doi.org/10.1016/j.ijcard.2018.01.058
Merlo M, Porcari A, Sinagra G (2018) The (ultra) sound of a burning heart: a matter of speckles. Int J Cardiol 259:132–133
Di Bella G, Gaeta M, Pingitore A, Oreto G, Zito C, Minutoli F, Anfuso C, Dattilo G, Lamari A, Coglitore S, Carerj S (2010) Myocardial deformation in acute myocarditis with normal left ventricular wall motion—a cardiac magnetic resonance and 2-dimensional strain echocardiographic study. Circ J 74:1205–1213
Aquaro GD, Perfetti M, Camastra G, Monti L, Dellegrottaglie S, Moro C, Pepe A, Todiere G, Lanzillo C, Scatteia A, Di Roma M, Pontone G, Perazzolo Marra M, Barison A, Di Bella G (2017) Cardiac MR with late gadolinium enhancement in acute myocarditis with preserved systolic function: ITAMY Study. J Am Coll Cardiol 70:1977–1987. https://doi.org/10.1016/j.jacc.2017.08.044
Caforio ALP, Pankuweit S, Arbustini E, Basso C, Gimeno-Blanes J, Felix SB, Fu M, Helio T, Heymans S, Jahns R, Klingel K, Linhart A, Maisch B, McKenna W, Mogensen J, Pinto YM, Ristic A, Schultheiss H-P, Seggewiss H, Tavazzi L, Thiene G, Yilmaz A, Charron P, Elliott PM (2648d) Current state of knowledge on aetiology, diagnosis, management, and therapy of myocarditis: a position statement of the European Society of Cardiology Working Group on Myocardial and Pericardial Diseases. Eur Heart J 34(2636–48):2648a–2648d. https://doi.org/10.1093/eurheartj/eht210
Sinagra G, Anzini M, Pereira NL, Bussani R, Finocchiaro G, Bartunek J, Merlo M (2016) Myocarditis in clinical practice. Mayo Clin Proc 91:1256–1266. https://doi.org/10.1016/j.mayocp.2016.05.013
Heymans S, Eriksson U, Lehtonen J, Cooper LTJ (2016) The quest for new approaches in myocarditis and inflammatory cardiomyopathy. J Am Coll Cardiol 68:2348–2364. https://doi.org/10.1016/j.jacc.2016.09.937
Friedrich MG, Sechtem U, Schulz-Menger J, Holmvang G, Alakija P, Cooper LT, White JA, Abdel-Aty H, Gutberlet M, Prasad S, Aletras A, Laissy J-P, Paterson I, Filipchuk NG, Kumar A, Pauschinger M, Liu P (2009) Cardiovascular magnetic resonance in myocarditis: a JACC White Paper. J Am Coll Cardiol 53:1475–1487. https://doi.org/10.1016/j.jacc.2009.02.007
Imazio M, Brucato A, Barbieri A, Ferroni F, Maestroni S, Ligabue G, Chinaglia A, Cumetti D, Della Casa G, Bonomi F, Mantovani F, Di Corato P, Lugli R, Faletti R, Leuzzi S, Bonamini R, Modena MG, Belli R (2013) Good prognosis for pericarditis with and without myocardial involvement: results from a multicenter, prospective cohort study. Circulation 128:42–49. https://doi.org/10.1161/CIRCULATIONAHA.113.001531
Buiatti A, Merlo M, Pinamonti B, De Biasio M, Bussani R, Sinagra G (2013) Clinical presentation and long-term follow-up of perimyocarditis. J Cardiovasc Med (Hagerstown) 14:235–241. https://doi.org/10.2459/JCM.0b013e328351da6e
Rösner A, Barbosa D, Aarsæther E, Kjønås D, Schirmer H, D’Hooge J (2015) The influence of Frame rate on two-dimensional speckle-tracking strain measurements: a study on silico-simulated models and images recorded in patients. Eur Heart J Cardiovasc Imaging. https://doi.org/10.1093/ehjci/jev058
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, Flachskampf FA, Foster E, Goldstein SA, Kuznetsova T, Lancellotti P, Muraru D, Picard MH, Rietzschel ER, Rudski L, Spencer KT, Tsang W, Voigt J-U (2015) Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging 16:233–270. https://doi.org/10.1093/ehjci/jev014
Voigt JU, Pedrizzetti G, Lysyansky P, Marwick TH, Houle H, Baumann R, Pedri S, Ito Y, Abe Y, Metz S, Song JH, Hamilton J, Sengupta PP, Kolias TJ, d’Hooge J, Aurigemma GP, Thomas JD, Badano LP (2015) Definitions for a common standard for 2D speckle tracking echocardiography: consensus document of the EACVI/ASE/Industry Task Force to standardize deformation imaging. Eur Heart J Cardiovasc Imaging. https://doi.org/10.1093/ehjci/jeu184
Badano LP, Kolias TJ, Muraru D, Abraham TP, Aurigemma G, Edvardsen T, D’Hooge J, Donal E, Fraser AG, Marwick T, Mertens L, Popescu BA, Sengupta PP, Lancellotti P, Thomas JD, Voigt JU (2018) Standardization of left atrial, right ventricular, and right atrial deformation imaging using two-dimensional speckle tracking echocardiography: a consensus document of the EACVI/ASE/Industry Task Force to standardize deformation imaging. Eur Heart J Cardiovasc Imaging. https://doi.org/10.1093/ehjci/jey042
Sekhon JS (2011) Multivariate and propensity score matching software with automated balance optimization: the matching package for R. J Stat Softw. https://doi.org/10.18637/jss.v042.i07
Walter SD, Eliasziw M, Donner A (1998) Sample size and optimal designs for reliability studies. Stat Med 17:101–110
Truong VT, Safdar KS, Kalra DK, Gao X, Ambach S, Taylor MD, Moore R, Taylor RJ, Germann J, Toro-Salazar O, Jefferies JL, Bartone C, Raman SV, Ngo T, Mazur W (2017) Cardiac magnetic resonance tissue tracking in right ventricle: feasibility and normal values. Magn Reson Imaging 38:189–195. https://doi.org/10.1016/j.mri.2017.01.007
Grani C, Eichhorn C, Biere L, Murthy VL, Agarwal V, Kaneko K, Cuddy S, Aghayev A, Steigner M, Blankstein R, Jerosch-Herold M, Kwong RY (2017) Prognostic value of cardiac magnetic resonance tissue characterization in risk stratifying patients with suspected myocarditis. J Am Coll Cardiol 70:1964–1976. https://doi.org/10.1016/j.jacc.2017.08.050
Ferreira VM, Piechnik SK, Dall’Armellina E, Karamitsos TD, Francis JM, Ntusi N, Holloway C, Choudhury RP, Kardos A, Robson MD, Friedrich MG, Neubauer S (2013) T(1) mapping for the diagnosis of acute myocarditis using CMR: comparison to T2-weighted and late gadolinium enhanced imaging. JACC Cardiovasc Imaging 6:1048–1058. https://doi.org/10.1016/j.jcmg.2013.03.008
Bohnen S, Radunski UK, Lund GK, Kandolf R, Stehning C, Schnackenburg B, Adam G, Blankenberg S, Muellerleile K (2015) Performance of T1 and T2 mapping cardiovascular magnetic resonance to detect active myocarditis in patients with recent-onset heart failure. Circ Cardiovasc Imaging. https://doi.org/10.1161/CIRCIMAGING.114.003073
Merlo M, Mase M, Vitrella G, Belgrano M, Faganello G, Di Giusto F, Boscutti A, Gobbo M, Gigli M, Altinier A, Lesizza P, Barbati G, Ramani F, De Luca A, Morea G, Cova MA, Stolfo D, Sinagra G (2018) Usefulness of addition of magnetic resonance imaging to echocardiographic imaging to predict left ventricular reverse remodeling in patients with nonischemic cardiomyopathy. Am J Cardiol. https://doi.org/10.1016/j.amjcard.2018.04.017
Baeßler B, Schaarschmidt F, Dick A, Michels G, Maintz D, Bunck AC (2016) Diagnostic implications of magnetic resonance feature tracking derived myocardial strain parameters in acute myocarditis. Eur J Radiol. https://doi.org/10.1016/j.ejrad.2015.11.023
Schmidt B, Dick A, Treutlein M, Schiller P, Bunck AC, Maintz D, Baessler B (2017) Intra- and inter-observer reproducibility of global and regional magnetic resonance feature tracking derived strain parameters of the left and right ventricle. Eur J Radiol 89:97–105. https://doi.org/10.1016/j.ejrad.2017.01.025
Schuster A, Morton G, Hussain ST, Jogiya R, Kutty S, Asrress KN, Makowski MR, Bigalke B, Perera D, Beerbaum P, Nagel E (2013) The intra-observer reproducibility of cardiovascular magnetic resonance myocardial feature tracking strain assessment is independent of field strength. Eur J Radiol 82:296–301. https://doi.org/10.1016/j.ejrad.2012.11.012
Bianco CM, Farjo PD, Ghaffar YA, Sengupta PP (2019) Myocardial mechanics in patients with normal LVEF and diastolic dysfunction. JACC Cardiovasc Imaging. https://doi.org/10.1016/j.jcmg.2018.12.035
Biering-Sorensen T, Biering-Sorensen SR, Olsen FJ, Sengelov M, Jorgensen PG, Mogelvang R, Shah AM, Jensen JS (2017) Global longitudinal strain by echocardiography predicts long-term risk of cardiovascular morbidity and mortality in a low-risk general population: the Copenhagen City Heart Study. Circ Cardiovasc Imaging. https://doi.org/10.1161/CIRCIMAGING.116.005521
André F, Stock FT, Riffel J, Giannitsis E, Steen H, Scharhag J, Katus HA, Buss SJ (2016) Incremental value of cardiac deformation analysis in acute myocarditis: a cardiovascular magnetic resonance imaging study. Int J Cardiovasc Imaging. https://doi.org/10.1007/s10554-016-0878-0
Anzini M, Merlo M, Sabbadini G, Barbati G, Finocchiaro G, Pinamonti B, Salvi A, Perkan A, Di Lenarda A, Bussani R, Bartunek J, Sinagra G (2013) Long-term evolution and prognostic stratification of biopsy-proven active myocarditis. Circulation 128:2384–2394. https://doi.org/10.1161/CIRCULATIONAHA.113.003092
Grun S, Schumm J, Greulich S, Wagner A, Schneider S, Bruder O, Kispert E-M, Hill S, Ong P, Klingel K, Kandolf R, Sechtem U, Mahrholdt H (2012) Long-term follow-up of biopsy-proven viral myocarditis: predictors of mortality and incomplete recovery. J Am Coll Cardiol 59:1604–1615. https://doi.org/10.1016/j.jacc.2012.01.007
Taylor RJ, Moody WE, Umar F, Edwards NC, Taylor TJ, Stegemann B, Townend JN, Hor KN, Steeds RP, Mazur W, Leyva F (2015) Myocardial strain measurement with feature-tracking cardiovascular magnetic resonance: normal values. Eur Heart J Cardiovasc Imaging 16:871–881. https://doi.org/10.1093/ehjci/jev006
Andre F, Steen H, Matheis P, Westkott M, Breuninger K, Sander Y, Kammerer R, Galuschky C, Giannitsis E, Korosoglou G, Katus HA, Buss SJ (2015) Age- and gender-related normal left ventricular deformation assessed by cardiovascular magnetic resonance feature tracking. J Cardiovasc Magn Reson 17:25. https://doi.org/10.1186/s12968-015-0123-3
Augustine D, Lewandowski AJ, Lazdam M, Rai A, Francis J, Myerson S, Noble A, Becher H, Neubauer S, Petersen SE, Leeson P (2013) Global and regional left ventricular myocardial deformation measures by magnetic resonance feature tracking in healthy volunteers: comparison with tagging and relevance of gender. J Cardiovasc Magn Reson 15:8. https://doi.org/10.1186/1532-429X-15-8
Acknowledgement
We would like to thank Fondazione CRTrieste, Fondazione CariGO, Fincantieri and all the healthcare professionals for the continuous support to the clinical management of patients affected by cardiomyopathies, followed in Heart Failure Outpatient Clinic of Trieste, and their families.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
392_2019_1577_MOESM1_ESM.docx
Supplementary material consists of statistical analysis of an age and gender-matched sample of confirmed AM compared to a healthy controls (Table S1), cut-off values for biventricular strain (Table S2), intraoperator and interoperator interclass correlation coefficient (Table S3). (DOCX 16 kb)
Rights and permissions
About this article
Cite this article
Porcari, A., Merlo, M., Crosera, L. et al. Strain analysis reveals subtle systolic dysfunction in confirmed and suspected myocarditis with normal LVEF. A cardiac magnetic resonance study. Clin Res Cardiol 109, 869–880 (2020). https://doi.org/10.1007/s00392-019-01577-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-019-01577-w