Abstract
Background
Choroidal thickness is associated with several cardiovascular parameters in case–control studies including patients with manifest disease. So far, it was unclear whether underlying cardiovascular risk factors or the continuum of heart failure may lead to alterations of the choroid. Therefore, our hypothesis was to test in a population-based study, whether choroidal thickness is associated with cardiovascular risk factors and heart disease.
Methods
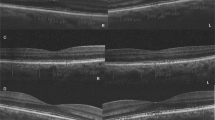
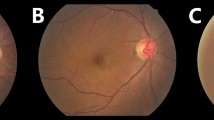
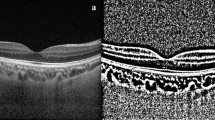
A population-based cross-sectional study was carried out in Germany. A comprehensive medical examination including assessment of cardiovascular risk factors, echocardiography and ophthalmological examinations with spectral-domain optical coherence tomography of the choroid was performed. Subfoveal choroidal thickness as well as left ventricular ejection fraction (LVEF) and a surrogate marker for left ventricular end-diastolic pressure (E/e’) were measured. Linear regression analyses were carried out to determine the relationship between subfoveal choroidal thickness and age, sex, body mass index, systolic blood pressure, dyslipidemia, HbA1c level, hematocrit, estimated glomerular filtration rate (eGFR), LVEF, E/e’ and left ventricular mass index adjusted for ocular parameters.
Results
1.742 subjects (48% females) with a mean age 59.3 ± 10.6 years were included in this study. Mean subfoveal thickness was 252 ± 77 µm (right eyes) and 255 ± 77 µm (left eyes). Unadjusted linear regression analysis revealed that subfoveal choroidal thickness is associated with sex, age, systolic blood pressure, hematocrit, eGFR, left ventricular end-diastolic pressure, left ventricular mass index (all p < 0.001) and dyslipidemia (p = 0.009). Adjusted linear regression only revealed age as associated parameter (p < 0.001).
Conclusions
We did find evidence for an association between subfoveal choroidal thickness and cardiovascular risk factors which was mediated by aging.
Graphic abstract



Similar content being viewed by others
References
Ahmad M, Kaszubski PA, Cobbs L, Reynolds H, Smith RT (2017) Choroidal thickness in patients with coronary artery disease. PLoS One 12(6):e0175691. https://doi.org/10.1371/journal.pone.0175691
Ahn SJ, Woo SJ, Park KH (2014) Retinal and choroidal changes with severe hypertension and their association with visual outcome. Invest Ophthalmol Vis Sci 55(12):7775–7785. https://doi.org/10.1167/iovs.14-14915
Akay F, Gundogan FC, Yolcu U, Toyran S, Uzun S (2016) Choroidal thickness in systemic arterial hypertension. Eur J Ophthalmol 26(2):152–157. https://doi.org/10.5301/ejo.5000675
Akcay BI, Kardes E, Macin S, Unlu C, Ozgurhan EB, Macin A, Bozkurt TK, Ergin A, Surmeli R (2016) Evaluation of subfoveal choroidal thickness in internal carotid artery stenosis. J Ophthalmol 2016:5296048. https://doi.org/10.1155/2016/5296048
Altinkaynak H, Kara N, Sayin N, Gunes H, Avsar S, Yazici AT (2014) Subfoveal choroidal thickness in patients with chronic heart failure analyzed by spectral-domain optical coherence tomography. Curr Eye Res 39(11):1123–1128. https://doi.org/10.3109/02713683.2014.898310
Pekel G, Dogu MH, Keskin A, Acer S, Yagci R, Kasikci A, Cetin EN (2015) Subfoveal choroidal thickness is associated with blood hematocrit level. Ophthalmologica 234(1):55–59. https://doi.org/10.1159/000433449
Tan KA, Gupta P, Agarwal A, Chhablani J, Cheng CY, Keane PA, Agrawal R (2016) State of science: choroidal thickness and systemic health. Surv Ophthalmol 61(5):566–581. https://doi.org/10.1016/j.survophthal.2016.02.007
Sansom LT, Suter CA, McKibbin M (2016) The association between systolic blood pressure, ocular perfusion pressure and subfoveal choroidal thickness in normal individuals. Acta Ophthalmol 94(2):e157–158. https://doi.org/10.1111/aos.12794
Wei WB, Xu L, Jonas JB, Shao L, Du KF, Wang S, Chen CX, Xu J, Wang YX, Zhou JQ, You QS (2013) Subfoveal choroidal thickness: the Beijing Eye Study. Ophthalmology 120(1):175–180. https://doi.org/10.1016/j.ophtha.2012.07.048
Gupta P, Jing T, Marziliano P, Cheung CY, Baskaran M, Lamoureux EL, Wong TY, Cheung CM, Cheng CY (2015) Distribution and determinants of choroidal thickness and volume using automated segmentation software in a population-based study. Am J Ophthalmol 159(2):293–301.e293. https://doi.org/10.1016/j.ajo.2014.10.034
Hohn R, Kottler U, Peto T, Blettner M, Munzel T, Blankenberg S, Lackner KJ, Beutel M, Wild PS, Pfeiffer N (2015) The ophthalmic branch of the Gutenberg Health Study: study design, cohort profile and self-reported diseases. PLoS One 10(3):e0120476. https://doi.org/10.1371/journal.pone.0120476
Shao L, Xu L, Chen CX, Yang LH, Du KF, Wang S, Zhou JQ, Wang YX, You QS, Jonas JB, Wei WB (2013) Reproducibility of subfoveal choroidal thickness measurements with enhanced depth imaging by spectral-domain optical coherence tomography. Invest Ophthalmol Vis Sci 54(1):230–233. https://doi.org/10.1167/iovs.12-10351
Rahman W, Chen FK, Yeoh J, Patel P, Tufail A, Da Cruz L (2011) Repeatability of manual subfoveal choroidal thickness measurements in healthy subjects using the technique of enhanced depth imaging optical coherence tomography. Invest Ophthalmol Vis Sci 52(5):2267–2271. https://doi.org/10.1167/iovs.10-6024
Spaide RF, Koizumi H, Pozzoni MC (2008) Enhanced depth imaging spectral-domain optical coherence tomography. Am J Ophthalmol 146(4):496–500. https://doi.org/10.1016/j.ajo.2008.05.032
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF 3rd, Feldman HI, Kusek JW, Eggers P, Van Lente F, Greene T, Coresh J (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, Flachskampf FA, Foster E, Goldstein SA, Kuznetsova T, Lancellotti P, Muraru D, Picard MH, Rietzschel ER, Rudski L, Spencer KT, Tsang W, Voigt JU (2015) Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr 28(1):1–39.e14. https://doi.org/10.1016/j.echo.2014.10.003
Nagueh SF, Smiseth OA, Appleton CP, Byrd BF 3rd, Dokainish H, Edvardsen T, Flachskampf FA, Gillebert TC, Klein AL, Lancellotti P, Marino P, Oh JK, Popescu BA, Waggoner AD (2016) Recommendations for the evaluation of left ventricular diastolic function by echocardiography: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr 29(4):277–314. https://doi.org/10.1016/j.echo.2016.01.011
Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JG, Coats AJ, Falk V, Gonzalez-Juanatey JR, Harjola VP, Jankowska EA, Jessup M, Linde C, Nihoyannopoulos P, Parissis JT, Pieske B, Riley JP, Rosano GM, Ruilope LM, Ruschitzka F, Rutten FH, van der Meer P (2016) 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: the task force for the diagnosis and treatment of acute and chronic heart failure of the european society of cardiology (ESC). Developed with the special contribution of the heart failure association (HFA) of the ESC. Eur J Heart Fail 18(8):891–975. https://doi.org/10.1002/ejhf.592
Bursi F, Weston SA, Redfield MM, Jacobsen SJ, Pakhomov S, Nkomo VT, Meverden RA, Roger VL (2006) Systolic and diastolic heart failure in the community. JAMA 296(18):2209–2216. https://doi.org/10.1001/jama.296.18.2209
Lam CSP, Gamble GD, Ling LH, Sim D, Leong KTG, Yeo PSD, Ong HY, Jaufeerally F, Ng TP, Cameron VA, Poppe K, Lund M, Devlin G, Troughton R, Richards AM, Doughty RN (2018) Mortality associated with heart failure with preserved vs. reduced ejection fraction in a prospective international multi-ethnic cohort study. Eur Heart J. https://doi.org/10.1093/eurheartj/ehy005
de Boer RA, Nayor M, deFilippi CR, Enserro D, Bhambhani V, Kizer JR, Blaha MJ, Brouwers FP, Cushman M, Lima JAC, Bahrami H, van der Harst P, Wang TJ, Gansevoort RT, Fox CS, Gaggin HK, Kop WJ, Liu K, Vasan RS, Psaty BM, Lee DS, Hillege HL, Bartz TM, Benjamin EJ, Chan C, Allison M, Gardin JM, Januzzi JL Jr, Shah SJ, Levy D, Herrington DM, Larson MG, van Gilst WH, Gottdiener JS, Bertoni AG, Ho JE (2018) Association of cardiovascular biomarkers with incident heart failure with preserved and reduced ejection fraction. JAMA Cardiol. https://doi.org/10.1001/jamacardio.2017.4987
Desai A, Fang JC (2008) Heart failure with preserved ejection fraction: hypertension, diabetes, obesity/sleep apnea, and hypertrophic and infiltrative cardiomyopathy. Heart Fail Clin 4(1):87–97. https://doi.org/10.1016/j.hfc.2007.11.001
Park JY, Kim BG, Hwang JH, Kim JS (2017) Choroidal thickness in and outside of vascular arcade in healthy eyes using spectral-domain optical coherence tomography. Invest Ophthalmol Vis Sci 58(13):5827–5837. https://doi.org/10.1167/iovs.17-22581
Gupta T, Saini N, Arora J, Sahni D (2017) Age-related changes in the chorioretinal junction: an immunohistochemical study. J Histochem Cytochem 65(10):567–577. https://doi.org/10.1369/0022155417726507
Gottdiener JS, Bednarz J, Devereux R, Gardin J, Klein A, Manning WJ, Morehead A, Kitzman D, Oh J, Quinones M, Schiller NB, Stein JH, Weissman NJ (2004) American society of echocardiography recommendations for use of echocardiography in clinical trials. J Am Soc Echocardiogr 17(10):1086–1119. https://doi.org/10.1016/j.echo.2004.07.013
Xu J, Xu L, Du KF, Shao L, Chen CX, Zhou JQ, Wang YX, You QS, Jonas JB, Wei WB (2013) Subfoveal choroidal thickness in diabetes and diabetic retinopathy. Ophthalmology 120(10):2023–2028. https://doi.org/10.1016/j.ophtha.2013.03.009
Gupta P, Thakku SG, Sabanayagam C, Tan G, Agrawal R, Cheung CMG, Lamoureux EL, Wong TY, Cheng CY (2017) Characterisation of choroidal morphological and vascular features in diabetes and diabetic retinopathy. Br J Ophthalmol 101(8):1038–1044. https://doi.org/10.1136/bjophthalmol-2016-309366
Schuster AK, Steinmetz P, Forster TM, Schlichtenbrede FC, Harder BC, Jonas JB (2014) Choroidal thickness in nonarteritic anterior ischemic optic neuropathy. Am J Ophthalmol 158(6):1342–1347.e1341. https://doi.org/10.1016/j.ajo.2014.09.008
Ikuno Y, Kawaguchi K, Nouchi T, Yasuno Y (2010) Choroidal thickness in healthy Japanese subjects. Invest Ophthalmol Vis Sci 51(4):2173–2176. https://doi.org/10.1167/iovs.09-4383
Eggebrecht L, Prochaska JH, Trobs SO, Schwuchow-Thonke S, Gobel S, Diestelmeier S, Schulz A, Arnold N, Panova-Noeva M, Koeck T, Rapp S, Gori T, Lackner KJ, Ten Cate H, Munzel T, Wild PS (2019) Direct oral anticoagulants and vitamin K antagonists are linked to differential profiles of cardiac function and lipid metabolism. Clin Res Cardiol. https://doi.org/10.1007/s00392-018-1408-y
Hirschberg K, Reinhart M, Mereles D, Uhlmann L, Andre F, Riffel J, Ochs M, Katus HA (2019) Echocardiographic calcification score in patients with low/intermediate cardiovascular risk. Clin Res Cardiol 108(2):194–202. https://doi.org/10.1007/s00392-018-1343-y
Fu M, Ahrenmark U, Berglund S, Lindholm CJ, Lehto A, Broberg AM, Tasevska-Dinevska G, Wikstrom G, Agard A, Andersson B (2017) Adherence to optimal heart rate control in heart failure with reduced ejection fraction: insight from a survey of heart rate in heart failure in Sweden (HR-HF study). Clin Res Cardiol 106(12):960–973. https://doi.org/10.1007/s00392-017-1146-6
Usui S, Ikuno Y, Akiba M, Maruko I, Sekiryu T, Nishida K, Iida T (2012) Circadian changes in subfoveal choroidal thickness and the relationship with circulatory factors in healthy subjects. Invest Ophthalmol Vis Sci 53(4):2300–2307. https://doi.org/10.1167/iovs.11-8383
Acknowledgements
The Gutenberg Health Study is funded through the government of Rhineland-Palatinate („Stiftung Rheinland-Pfalz für Innovation“, contract AZ 961-386261/733), the research programs “Wissen schafft Zukunft” and “Center for Translational Vascular Biology (CTVB)” of the Johannes Gutenberg-University of Mainz, and its contract with Boehringer Ingelheim and PHILIPS Medical Systems, including an unrestricted grant for the Gutenberg Health Study. Philipp S. Wild is funded by the Federal Ministry of Education and Research (BMBF 01EO1503) and he is PI of the German Center for Cardiovascular Research (DZHK). Pfeiffer N receives financial support by Novartis, Ivantis, Santen, Thea, Boehringer Ingelheim Deutschland GmbH & Co. KG, Alcon, Sanoculis. Schuster AK holds the professorship for ophthalmic healthcare research donated by „Stiftung Auge“and financed by „Deutsche Ophthalmologische Gesellschaft“and „Berufsverband der Augenärzte Deutschlands e.V.“ All other authors: none. We thank all study participants for their willingness to provide data for this research project and we are indebted to all coworkers for their enthusiastic commitment.
Funding
Schuster AK received research funding from Bayer Vital, Novartis and Heidelberg Engineering; Pfeiffer N: receives financial support and grants by Novartis, Ivantis, Santen, Thea, Boehringer Ingelheim Deutschland GmbH & Co. KG, Alcon, Sanoculis; Nickels S received reimbursement of travel expenses from Novartis Pharma GmbH; Wild PS: received research grants from Boehringer Ingelheim Deutschland GmbH & Co. KG, Daiichi Sankyo Deutschland GmbH, Bayer HealthCare-Bayer-Vital GmbH, Portavita BV, Sanofi-Aventis Deutschland GmbH, the German Ministry of Research and the Ministry of Health of Rhineland-Palatinate; Münzel T: received speakers honorary from Boehringer Ingelheim Deutschland GmbH & Co. KG, Servier Deutschland GmbH, Actavis Deutschland GmbH, Berlin Chemie Deutschland and currently research grants from the German Ministry of Research and the government of Rhineland-Palatinate; all other authors: none.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Ethical statement
The study was approved by the ethics committee (Ethics Commission of the State Chamber of Physicians of Rhineland-Palatinate).
Informed consent
According to the tenets of the Declaration of Helsinki, written informed consent was obtained from all participants prior to entering the study.
Additional information
Pfeiffer N. and Wild P.S. are senior authors.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Schuster, A.K., Leuschner, A., Feretos, C. et al. Choroidal thickness is associated with cardiovascular risk factors and cardiac health: the Gutenberg Health Study. Clin Res Cardiol 109, 172–182 (2020). https://doi.org/10.1007/s00392-019-01498-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-019-01498-8