Abstract
Background
Sympathetic nervous system activation plays a pivotal role in obese patients with obstructive sleep apnea (OSA), contributing to increased cardiovascular risk. Epicardial adipose tissue (EAT) activates cardiac autonomic nervous system. Our main study objective was to investigate effects of these autonomic dysfunction factors on post-exercise heart rate recovery (HRR).
Methods
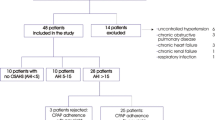
36 patients, referred for clinical assessment of obesity (BMI > 30 kg/m2), underwent overnight polysomnography, transthoracic echocardiography and cardiopulmonary exercise testing.
Results
Compared to non-OSA patients, OSA patients were older and displayed reduced body weight-indexed peak VO2. Cardiac output at peak exercise was similar among groups. Peak exercise arterio-venous oxygen content difference D[a-v]O2 was lower in OSA patients. In univariate linear analysis, age, AHI, EAT thickness, peak VO2 and diabetes were associated with blunted HRR. Multiple linear regression analysis showed that increased EAT thickness, AHI and diabetes were independently associated with lower HRR. For identical AHI value and diabetes status, HRR significantly decreased by 61.7% for every 1 mm increase of EAT volume (p = 0.011). If HRR was treated as a categorical variable, EAT [odds ratio (OR) 1.78 (95% confidence interval [CI] 1.19–2.66); p = 0.005], and type 2 diabetes [OR 8.97 (95% CI 1.16–69.10); p = 0.035] were the only independent predictors of blunted HRR.
Conclusions
Aerobic capacity and peak exercise D[a-v]O2 are impaired in obese OSA patients, suggesting abnormal peripheral oxygen extraction. EAT thickness is an independent marker of post-exercise HRR, which is a noninvasive marker of autonomic nerve dysfunction accompanying poor cardiovascular prognosis in obese patients.
Similar content being viewed by others
References
Guarino D, Nannipieri M, Iervasi G, Taddei S, Bruno RM (2017) The role of the autonomic nervous system in the pathophysiology of obesity. Front Physiol 8:665. https://doi.org/10.3389/fphys.2017.00665
Baguet JP, Barone-Rochette G, Tamisier R, Levy P, Pépin JL (2012) Mechanisms of cardiac dysfunction in obstructive sleep apnea. Nat Rev Cardiol 9:679–688. https://doi.org/10.1038/nrcardio.2012.141
Parati G, Lombardi C, Castagna F, Mattaliano P, Filardi PP, Agostoni P, Italian Society of Cardiology (SIC) (2016) Heart failure and sleep disorders. Nat Rev Cardiol 13:389–403. https://doi.org/10.1038/nrcardio.2016.71
Floras JS (2018) Sleep apnea and cardiovascular disease: an enigmatic risk factor. Circ Res 122:1741–1764. https://doi.org/10.1161/CIRCRESAHA.118.310783
Tafelmeier M, Weizenegger T, Ripfel S et al (2018) Postoperative complications after elective coronary artery bypass grafting surgery in patients with sleep-disordered breathing. Clin Res Cardiol 107:1148–1159. https://doi.org/10.1007/s00392-018-1289-0
Reuter H, Herkenrath S, Treml M et al (2018) Sleep-disordered breathing in patients with cardiovascular diseases cannot be detected by ESS, STOP-BANG, and Berlin questionnaires. Clin Res Cardiol 107:1071–1078. https://doi.org/10.1007/s00392-018-1282-7
Omran H, Bitter T, Horstkotte D, Oldenburg O, Fox H (2018) Characteristics and circadian distribution of cardiac arrhythmias in patients with heart failure and sleep-disordered breathing. Clin Res Cardiol 107:965–974. https://doi.org/10.1007/s00392-018-1269-4
Desteghe L, Hendriks JML, McEvoy RD et al (2018) The why, when and how to test for obstructive sleep apnea in patients with atrial fibrillation. Clin Res Cardiol 107:617–631. https://doi.org/10.1007/s00392-018-1248-9
Strotmann J, Fox H, Bitter T et al (2018) Characteristics of sleep-disordered breathing in patients with atrial fibrillation and preserved left ventricular ejection fraction. Clin Res Cardiol 107:120–129. https://doi.org/10.1007/s00392-017-1163-5
Nakamura S, Asai K, Kubota Y, Murai K et al (2015) Impact of sleep-disordered breathing and efficacy of positive airway pressure on mortality in patients with chronic heart failure and sleep-disordered breathing: a meta-analysis. Clin Res Cardiol 104:208–216. https://doi.org/10.1007/s00392-014-0774-3
Cholidou KG, Manali ED, Kapsimalis F et al (2015) Heart rate recovery post 6-minute walking test in obstructive sleep apnea: cycle ergometry versus 6-minute walking test in OSA patients. Clin Res Cardiol 103:805–815. https://doi.org/10.1007/s00392-014-0721-3
Okutucu S, Karakulak UN, Aytemir K, Oto A (2011) Heart rate recovery: a practical clinical indicator of abnormal cardiac autonomic function. Expert Rev Cardiovasc Ther 9:1417–1430. https://doi.org/10.1586/erc.11.149
Qiu S, Cai X, Sun Z et al (2017) Heart rate recovery and risk of cardiovascular events and all-cause mortality: a meta-analysis of prospective cohort studies. J Am Heart Assoc 6:e005505. https://doi.org/10.1161/JAHA.117.005505
Arab C, Vanderlei LCM, da Silva Paiva L et al (2018) Cardiac autonomic modulation impairments in advanced breast cancer patients. Clin Res Cardiol 107:924–936. https://doi.org/10.1007/s00392-018-1264-9
Maeder MT, Ammann P, Schoch OD et al (2010) Determinants of postexercise heart rate recovery in patients with the obstructive sleep apnea syndrome. Chest 137:310–317. https://doi.org/10.1378/chest.09-1424
Kline CE, Crowley EP, Ewing GB et al (2013) Blunted heart rate recovery is improved following exercise training in overweight adults with obstructive sleep apnea. Int J Cardiol 67:1610–1615. https://doi.org/10.1016/j.ijcard.2012.04.108
Gaborit B, Sengenes C, Ancel P, Jacquier A, Dutour A (2017) Role of epicardial adipose tissue in health and disease: a matter of fat? Compr Physiol 7:1051–1082. https://doi.org/10.1002/cphy.c160034
Kim MK, Tanaka K, Kim MJ et al (2010) Epicardial fat tissue: relationship with cardiorespiratory fitness in men. Med Sci Sports Exerc 42:463–469. https://doi.org/10.1249/MSS.0b013e3181b8b1f0
Sengul C, Duman D (2011) The association of epicardial fat thickness with blunted heart rate recovery in patients with metabolic syndrome. Tohoku J Exp Med 224:257–262
Akoumianakis I, Antoniades C (2017) The interplay between adipose tissue and the cardiovascular system: is fat always bad? Cardiovasc Res 113:999–1008. https://doi.org/10.1093/cvr/cvx111
Mariani S, Fiore D, Barbaro G et al (2013) Association of epicardial fat thickness with the severity of obstructive sleep apnea in obese patients. Int J Cardiol 167:2244–2249. https://doi.org/10.1016/j.ijcard.2012.06.011
Barone-Rochette G, Vivodtzev I, Tamisier R et al (2015) Left ventricular remodeling and epicardial fat volume in obese patients with severe obstructive sleep apnea treated by continuous positive airway pressure. Int J Cardiol 179:218–219. https://doi.org/10.1016/j.ijcard.2014.11.023
Mendelson M, Marillier M, Bailly S et al (2018) Maximal exercise capacity in patients with obstructive sleep apnoea syndrome: a systematic review and meta-analysis. Eur Respir J 51 Pii: 1702697. https://doi.org/10.1183/13993003.02697-2017
Hoyos CM, Melehan KL, Liu PY, Grunstein RR, Phillips CL (2015) Does obstructive sleep apnea cause endothelial dysfunction? A critical review of the literature. Sleep Med Rev 20:15–26. https://doi.org/10.1016/j.smrv.2014.06.003
Wang J, Yu W, Gao M, Zhang F, Gu C, Yu Y, Wei Y (2015) Impact of obstructive sleep apnea syndrome on endothelial function, arterial stiffening, and serum inflammatory markers: An updated meta-analysis and metaregression of 18 studies. J Am Heart Assoc 4:e002454. https://doi.org/10.1161/JAHA.115.002454
Gea J, Casadevall C, Pascual S, Orozco-Levi M, Barreiro E (2012) Respiratory diseases and muscle dysfunction. Expert Rev Respir Med 6:75–90. https://doi.org/10.1586/ers.11.81
Hargens TA, Guill SG, Zedalis D, Gregg JM, Nickols-Richardson SM, Herbert WG (2008) Attenuated heart rate recovery following exercise testing in overweight young men with untreated obstructive sleep apnea. Sleep 31:104–110
Zhou Q, Zhang L, Wang K et al (2014) Effect of interconnection between cervical vagus trunk, epicardial fat pad on sinus node function, and atrial fibrillation. Pacing Clin Electrophysiol 37:356–363. https://doi.org/10.1111/pace.12265
Parisi V, Rengo G, Perrone-Filardi P et al (2016) Increased epicardial adipose tissue volume correlates with cardiac sympathetic denervation in patients with heart failure. Circ Res 118:1244–1253. https://doi.org/10.1161/CIRCRESAHA.115.307765
Trayhurn P (2013) Hypoxia and adipose tissue function and dysfunction in obesity. Physiol Rev 93:1–21. https://doi.org/10.1152/physrev.00017.2012
Acknowledgements
This work was supported by a grant from the Clinical Research and Innovation Unit (DRCI) of the University Hospital of Martinique (2016).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no relationships that could be construed as a conflict of interest.
Additional information
Astrid Montfort and Jocelyn Inamo equally contributed to this work.
Rights and permissions
About this article
Cite this article
Monfort, A., Inamo, J., Fagour, C. et al. Epicardial fat accumulation is an independent marker of impaired heart rate recovery in obese patients with obstructive sleep apnea. Clin Res Cardiol 108, 1226–1233 (2019). https://doi.org/10.1007/s00392-019-01454-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-019-01454-6